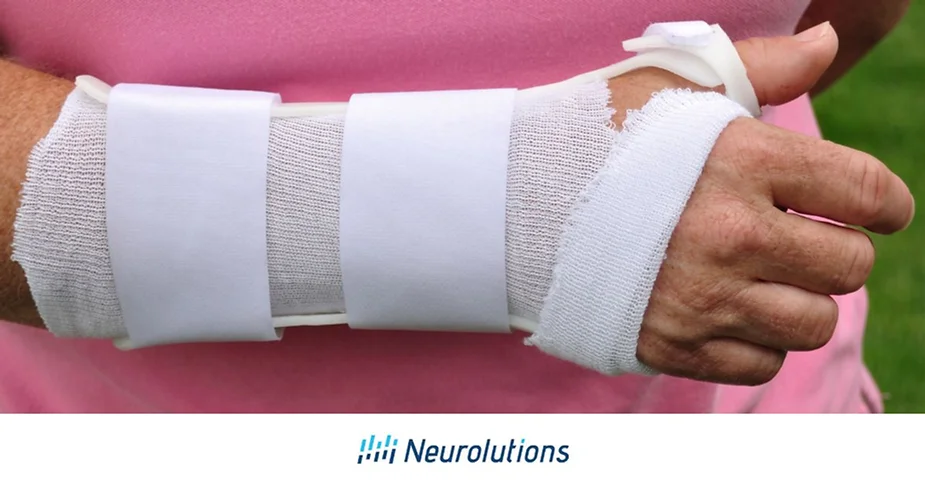
Orthotics are commonly used in stroke rehabilitation to increase arm stability, prevention of joint deformities and contractures, increase comfort and increase independence following a stroke and other neurological insults or diagnoses. Although some stroke survivors can be resistant to the use of orthotics due to a “bulky” feeling of fit, look, or price, the use of forearm/hand orthotics can be crucial in recovery. The use of orthotics, especially paired with functional use of the hand can be critical in early intervention of stroke rehabilitation. Not only can orthotics provide stability and alignment of the joints in the hand, wrist, and elbow by prevention of contractures, but they can also provide pain relief, compensate for the loss of sensation in the limb following a stroke, and at times help with swelling.
What is an Orthotic?
Webster’s dictionary defines orthotics as using “an artificial support or brace for the limb.” There are many kinds that can be used following a stroke. Upper extremity orthotics differ from lower extremity in use as more people are familiar with lower extremity braces for the knee and ankle or foot whether for stroke survivors or athletes alike as they provide stability for walking and balance.
In contrast, most hand orthotics are used in preparation for functional use by maintaining the position of the hand and not necessarily for use during an activity. Some orthotics, also known as “splints”, the types can be worn during functional activity, but many are used during rest, in preparation for activity by helping to combat spasticity or position the hand in our “normal” or “neutral” position.
How Do I Get a Hand or Arm Splint?
For many stroke survivors, an assessment with an occupational therapist is crucial for the recommendation of the proper splint or orthotic. There are many splints on the market, off the shelf and custom made but it is necessary to have the evaluation be completed by an occupational therapist, a certified hand therapist, or orthotist as many points are not appropriate for every patient following stroke and need to be properly fitted. Not only are the assessment required for a recommendation of the appropriate splint but also for a wear schedule and donning/doffing instructions. Hand splints differ from lower extremity splints in the wear schedule. Many hand splints are worn at night to provide a prolonged low-laid stretch at night, in direct contrast to lower extremity orthotics which are worn during ambulation and transfers.
Types of Arm and Hand Splints
Although there are many splints appropriate for the upper extremity following aas stroke, the following are the most commonly recommended:
Volar Resting Hand Splint
- Provides support under the hand and wrist providing a prolonged stretch in neutral positioning. Good for high and low tone.
Dynamic Stretching Splint
- Fitted with a crank which can be increased as tolerance to stretch increases. Used at both the wrist, elbow, or both. Requires fitting of an orthotists for custom wear.
Wrist Cockup Splint
- Provides stability at the wrist if weakness is present allowing for isolation of the digits during functional use.
Metacarpal Blocking Splint
- Allows for positioning of the knuckles in the proper placement for use of grasp/release.
Oval 8 Splint
- Provides stability at either the middle or furthest joint of the finger allowing for proper positioning in preparation for functional use.
Do I Need to See a Healthcare Professional After Getting My Orthotic?
After obtaining the appropriate splint, it is important to work with your therapist to allow for training and use of the splint. The orthotic does no good if it sits on a shelf or is not worn properly. It is also important to continually check the skin for any redness or rubbing which is common following a stroke. When the hand is static and sometimes with decreased sensation, repeated rubbing can occur causing skin breakdown.
It is also important to note that there are orthotics available on the market that aim to “break the tone” by placing the hand or wrist joint in hyperextension or flexion. Although these have been popular at times, it is important to note that research has now shown that these have no effect on tone management and can damage the limb.
For all orthotics, padding can be added as well as adjustments to the orthotic itself. Many splints or orthotics can be cleaned with soap and water and left to dry but always check the manufacturer’s recommendations for care recommendations. Needs can change over time as well as recovery continues, possibly changing recommendations in wear and use, therefore a “check-up” yearly in therapy is always a good idea.