Orthotics are commonly used in stroke rehabilitation to increase safety, stability, and independence following a stroke and other neurological insults or diagnoses. Although some can be resistant to the use of orthotics, they can be imperative to recovery and pathways to regaining mobility and hand use following one-sided/two-sided weakness or coordination deficits following a stroke. All research surrounding stroke indicates the importance of early mobility in stroke recovery. Using orthotics, especially when paired with the use of assistive devices, can allow for early mobility and focus on early intervention of stroke rehabilitation.
Webster’s dictionary defines orthotics as using “an artificial support or brace for the limb.” There are many kinds that can be used following a stroke. Not only can orthotics provide stability and alignment, but they can also provide pain relief, compensate for the loss of sensation in the limb following a stroke, and at times help with swelling.
Most Common Orthotics
Ankle Foot Orthosis (AFO)
Allows for stability and bracing from the ankle to the foot. Commonly used for foot drop (decreased foot flexion)
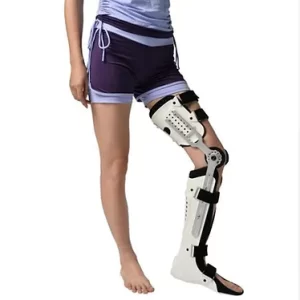
Knee Ankle Foot Orthosis (KAFO)
Allow for stability and bracing spanning from the knee to the ankle to the foot. Used commonly in the first stages of recovery for extra support with mobility.
Shoe Inserts (Orthotics)
Orthotics used only in the shoe under the foot to help provide high-level balance and alignment support. Thesee often times are referred to as “orthotics” and sometimes “UCBL’s”.
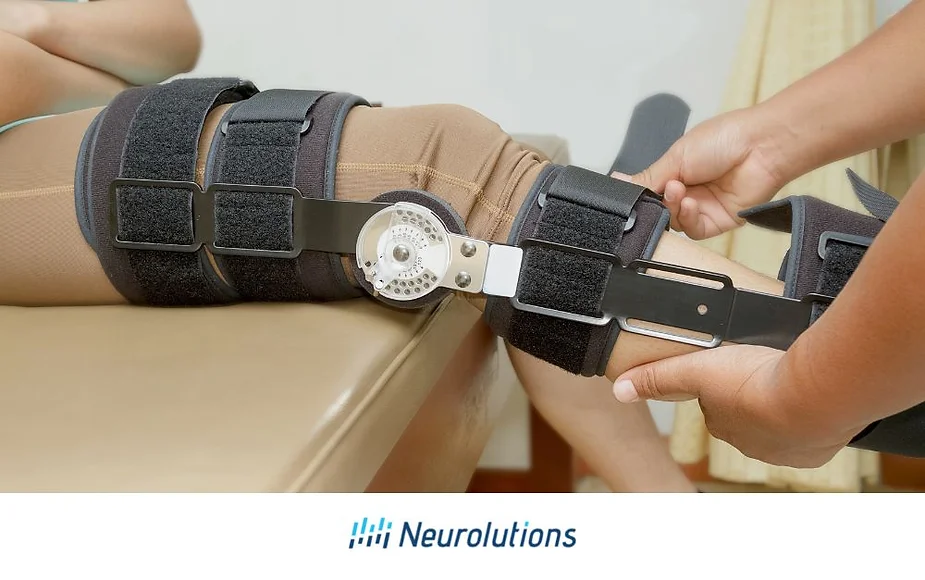
Knee Brace
Provides support and bracing at the knee to block buckling of the knee when standing or walking. Used commonly in the first stages of rehabilitation for stability and safety.
Orthotics, which provide stability can allow for the safe progression of mobility from the following:
- Static Sit to Standing
- Static Standing
- Static Standing with Reaching
- Stand Pivot Transfers
- Step Pivot Transfer
- In-Line Walking
- Dynamic Balance
- Walking with an Assistive Device
- Walking without an Assistive Device
Each of these activities is vital in working up to full mobility following a stroke. Using orthotics allows for the individual to focus on the steps or sequencing by providing stability to the weak joints and positioning the limb in the proper placement needed for walking or standing.
Foot Drop
Specifically, for survivors who experience foot drop caused by weakness of the “….muscles”. When foot drop occurs, the toes point down to the ground, causing a tripping hazard and impeding the ability to take a step safely causing immediate falls unless the individual is able to compensate with an over-exaggerated hip hike to bring the foot up and totally over a step. Exaggerated hip hiking is not an effective gait pattern and is unsustainable to continue with walking or transfers. The use of an AFO (ankle foot orthosis) can provide the stability at the ankle to stop foot drop. This allows the foot to remain in proper functional positioning during transfers and walking. The proper position increases safety and independence by decreasing the risk for falls.
Choosing the Right Orthotic
Choosing the right orthotic is important for stroke survivors who require support and stability for their limbs. Physical therapists and orthotists are the experts who can evaluate the need for orthotic use, and determine if customized or off-the-shelf orthotics are needed.
What is an Orthotist?
An orthotist is a healthcare professional who specializes in the design, fabrication, and fitting of orthotic devices. An orthotic device is a custom-made brace or splint that can be worn to support weakened joints or muscles, improve posture, and increase mobility. Orthotics are often used to help people recover from physical trauma such as stroke or injury. They can also be used for medical conditions such as cerebral palsy or arthritis. An orthotist will assess a patient’s condition and design an individualized treatment plan that includes the use of orthotic devices to help with recovery and rehabilitation.
Determining the Need for Orthotic Use
The use of orthotics may change throughout the recovery and rehabilitation process. After a stroke, a survivor may benefit from an orthotic that provides full support from the toe up to the knee. However, as strength and balance increase, the individual may require an orthotic that only provides support to the ankle. The physical therapist and orthotist work together to determine the client’s needs and may use off-the-shelf orthotics as a trial before customizing one.
Customized Orthotics
When a customized orthotic is required, an orthotist will either come to therapy and complete the consult or the survivor will meet with an orthotist at their clinic to take molds of the limb. The goal for a customized orthotic is to allow for the least cumbersome device and best fit.
The Importance of Consulting a Professional
It is important to consult a physical therapist or orthotist for orthotics rather than buying something off the shelf at a pharmacy or online. Off-the-rack orthotics are often made of thick fabrics that do not provide the required stability for most survivors. Physical therapists also guide the use of mobility aids for recovery and recommend progression to decrease the use of mobility aids.
Combining Orthosis and Mobility Aids
Orthotics provide stability for joints and help align the limb for proper positioning in preparation for mobility. However, they do not support the whole body for mobility. Mobility aids such as walkers, hemi-walkers, or canes are often paired with orthotics to aid in regaining mobility following a stroke.
Physical therapists and orthotists are the experts in evaluating the need for orthotic use and guiding the process. Choosing the right orthotic can help stroke survivors with balance and safe mobility, while also allowing for progress toward decreased use of mobility aids.
Caring for and Maintaining Orthotics
Orthotic Care
Since orthotics are ideally worn at all times throughout the day to allow for the greatest safety with transfers and mobility, general wear and tear will take place. It is best to keep the orthotics clean by washing them with regular soap and water and allowing air to dry overnight when not night-wearing. Sanitizing sprays can also help keep the orthotic clean and fresh. Many orthotic companies, especially when using customized orthotics come with cleaning and care instructions for the materials used. Please make sure you are following all manufacturing recommendations for cleaning and care. Due to wear and tear, breakage will take place. If a break occurs, contact your orthotists or physical therapist immediately to help with the process of fixing or ordering a new one as a break can impact safety and use.
Mobility Aid Care
When maintaining mobility aids such as walkers or canes, it is important to keep the handles and feet of the devices clear of “muck” and other items so that all parts of the device are free of clutter to allow for the greatest safety and for long use. Most insurances only pay for a new assistive device every five years unless there is a large change in medical status if they pay at all. Therefore, the device you have now may be with you for a long time, so take good care of it. If your handle grip for instance is starting to wear and tear, place tape around the tear prior to it ripping all the way before you can no longer use it.
Conclusion
Some stroke survivors have been known to be resistant to the use of orthotics or mobility aids for one of two reasons:
- They do not like how they make them look, making them look old, or
- They feel like using an orthotic or aide is a “crutch” and will not allow them to build strength on their own.
Both are false. Using a device does not make you more weak or sick. It is imperative to use both if needed following a stroke as the only intervention that allows for regaining function is actually completing tasks themselves and by getting weight-bearing opportunities to the legs in preparation for walking and transfers. Without the use of the devices, the survivor may not even be able to stand. A stroke is not the same as breaking your foot, which heals on its own in a cast without doing anything. A stroke requires active intervention for rehabilitation. If an orthotic is recommended, listen to this advice. Using one right after the stroke through recovery does not mean that it will be forever. Allow for this compensation, help allow for rehabilitation to regain strength and independence, and will help decrease dependence on devices over time in your journey to recovery.
References:
https://www.merriam-webster.com/