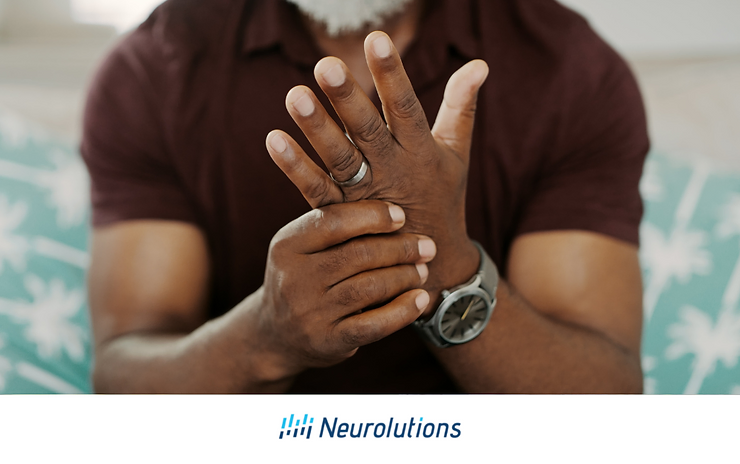
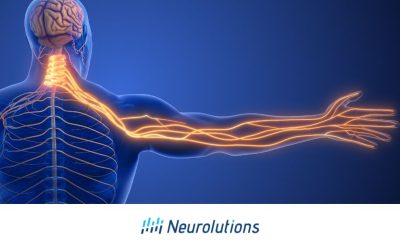
Muscle atrophy is the loss of muscle tissue or the thinning of a muscle. This can be due to multiple medical reasons, aging, malnutrition, or lack of physical activity, but muscle atrophy can specifically happen following a stroke. Muscle atrophy occurs secondary to a lack of nerve innervation in the muscle groups to the hemiparetic region of the body which has been affected.
Following a stroke, the best way to prevent muscle atrophy of the arm is by using the affected upper extremity. In some cases, muscle atrophy occurs due to disuse and not nerve disruption. Learned non-use begins immediately at the time of a stroke. The best prevention is to USE THE ARM!
How To Treat Muscle Atrophy?
The best way to prevent muscle atrophy is the use of the affected muscle groups. Prevention of upper extremity muscle atrophy following a stroke can look like the following::
1. Active Range Of Motion
An overwhelming amount of evidence supporting the use of massed practice and high repetition shows the most promise for regaining function of the upper extremity following a stroke. This speaks to the importance of continually trying new things to address hand weakness.
No matter the extent of your weakness or tone, it is imperative to make attempts to use your hand as much as you can. It is also very important to use your hand in high repetition circumstances, such as flipping over cards or stacking plastic cups. The more the better. Complete aerobic activity such as walking or traditional non-weighted exercise of the upper extremity. Talk to your physical or occupational therapist for further guidance for active range of motion and integration or greater use.
2. Passive Range Of Motion
If unable to produce an active range of motion, a home exercise program should include a passive range of motion to the muscles and joints. Passive range of motion exercises may help prevent deformities as well as sustain muscle integrity. Meanwhile, continue to address active movement and functional use of the arm as much as possible. Talk to your physical or occupational therapist for further guidance on the passive range of motion.
3. Integration Of The Arm Into Function By The Following Techniques
- Weight-bearing during activity- If unable to use the arm in the daily activities, place the affected hand on the top of the table or sink with the elbow extended while completing the activity. Weight-bearing helps elicit muscle stabilization, trunk stability, and scapular stability. Once weight bearing is achieved through the affected upper extremity, the stroke survivor can effectively aid the whole body during the activity, using the non-affected arm to complete the activity.
- Moving objects across a surface with the affected arm even if unable to fully grasp- If unable to use the arm in daily activities, the stroke survivor can use the arm in a gross motor-like fashion using the shoulder or elbow to hook on an object as well as pushing or pulling an object across a surface.
4. Use Of Technologies Such As Functional Electrical Stimulation, Robotics, Or Brain-Computer Interface To Help Provide Functional Movement Of The Upper Extremity If Unable To Do So For Themselves
The integration of technology such as functional electrical stimulation (FES), vibration, robotics, and brain-computer interface systems can help provide stimulation to the affected muscle groups to increase activation of muscle contraction in priming or preparation of functional use of the activity.
5. Prevention Of Pain
Being able to use and involve the affected upper extremity is highly dependent on the tolerance to involve and use the arm in all activities. As a generality, the stroke itself does not tend to cause pain in the weak arm. Rather, complications to the upper extremity following strokes such as contractures, edema, or subluxation (separation of the glenohumeral joint due to weakness in the arm) correlate with the pain.
When pain and edema impact the ability to use the affected arm, muscle atrophy will continue to develop because the arm is unable to integrate into activity or exercise. Edema techniques and appropriate support of the arm using an arm trough, a tray, pillows, and sometimes a well-constructed splint or brace can help maintain proper positioning of the joints and blood/fluid movement to the affected areas.
6. Medications
Medications prescribed by your neurologist can help with the improvement of muscle tone and reduce pain in the hands and arms, allowing for increased functional use and positioning of the arm, overall helping to ward off muscle atrophy. These anti-spasticity pharmaceuticals are taken orally, are locally injected, or can be delivered through an implantable pump. A physician that specializes in physical medicine and rehabilitation and some neurologists will be able to determine which options are best for your unique presentation.
Muscle atrophy prevention is not always a central focus of medical care or rehabilitation following a stroke. This condition can become more problematic and defined as time progresses post-stroke. Integration of the above techniques can be helpful in the prevention of the onset or severity of the affected upper extremity. Even if muscle atrophy is not a concern at this time, the above information can also be used to increase knowledge and understanding of techniques for upper extremity rehabilitation following a stroke. Talk to your rehabilitation team if you have concerns about muscle atrophy or disuse.
References:
Pedretti, Pendleton, Schultz-Krohn, Pedretti’s Occupational Therapy: Practice skills for Physical Dysfunction. Stl. Louis, MO Mosby/Elsevier, 2006.