Introduction: What is a Cerebellum Stroke?
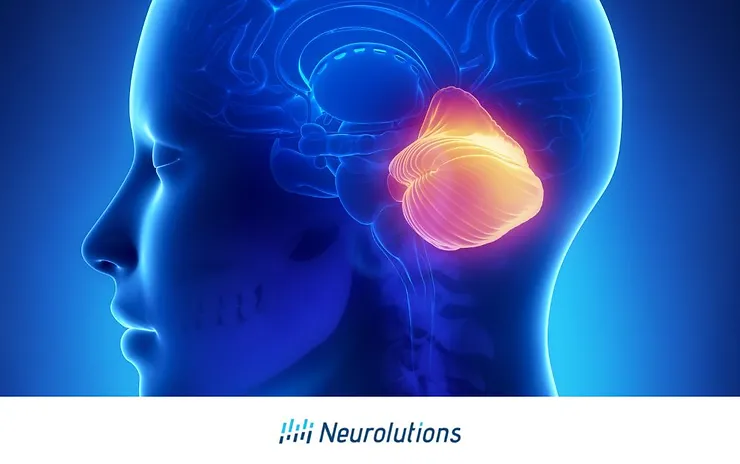
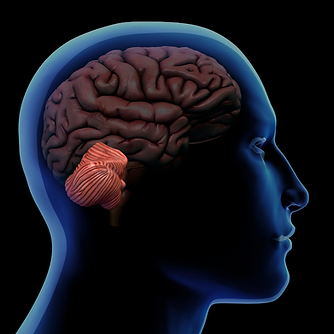
When a cerebellar artery occlusion occurs, this result is a stroke in the area of the cerebellum. The word cerebellum in Latin refers to “little brain.” The cerebellum is a small area of the brain and is located at the back of the brain near the brain stem, above and behind where the spinal cord attaches to the brain.
Most commonly, cerebellar strokes result in problems with coordination and ataxia. Cerebellar strokes are less common than other types of strokes. It is estimated that cerebellar strokes account for 1.5-10% of all strokes but evidence suggests that deaths related to cerebellar strokes range anywhere between 23-38%.
Stroke Causes and Risk Factors
Risk factors for cerebellar stroke include the same risk factors as all other strokes. Some of these risk factors include smoking, diabetes, high cholesterol, and high blood pressure. There is some evidence demonstrating an increased incidence of cerebellar stroke linked to alcohol measures or medication side effects compared to other types of strokes.
Genetic abnormalities also can be a cause of cerebellar strokes due to how the development of the brain occurs in utero, specifically in the area of the cerebellum and brainstem. In comparison to other strokes as well, cerebellar strokes may manifest with ataxia, vertigo, dysarthria, nausea, vomiting, and often a prominent headache compared with other strokes that may present with facial and one-sided weakness.
Consequences of Cerebellum Strokes
When a stroke occurs in the cerebellum, common symptoms or impairments that may occur are the following:
- Ataxia: decreased coordination of muscle movements (can be one-sided or whole body). Ataxia can also result in postural instability leading to balance problems.
- Lack of a “check” reflex: This is the inability to motion quickly to avoid running into something with the whole body or a portion of the body.
- Hypermetria: overshooting of a limb to a target
- Dyssynergia: voluntary movements that are broken up into the parts of the movement and appear jerky. This can cause problems in all motor movements and speech.
- Hypometria: undershooting of the limb to a target
- Adiadochokinesia: the inability to perform rapid alternating movements, such as movements of the hands in a rapid motion of flipping pancakes
- Loss of pain on the contralateral (opposite) side of the body
- Temperature sensitivity on the contralateral side of the body
- Ipsilateral loss of numbness on the face
- Dysphagia: difficulty swallowing foods or liquids
- Dysarthria: weakness of mouth muscles used for speaking causing difficulty talking
- Nystagmus: decreased coordination involuntary movement of the eyes in the up-down-back and forth or rotating direction. Nystagmus interferes with head control and adjustments required for balance.
Recovery from Cerebellum Strokes
Therapy can be very beneficial to help assist with recovery from a cerebellar stroke. Your physical therapist will assess how the cerebellar deficits have impacted all facets related to mobility, balance, muscle strength, and range of motion. Occupational therapists will evaluate how cerebellar impairments such as ataxia impact activities such as writing, opening containers or applying toothpaste to toothbrushes.
Stabilization techniques such as leaving the elbow on the table or against the body can help improve control or limb movement. In all honesty, coordination impairments can be difficult but activities to facilitate motor learning and obtaining proximal stability increase control of reflexes. Modalities such as electric stimulation and the use of moist heat can be used in conjunction with other interventions such as weight-bearing exercises when focusing on the participation of ADLs (activities of daily living) and mobility.
The use of adaptive equipment to lessen the likelihood of errors can also be helpful. This can range from off-the-shelf items such as using a non-spill water bottle with a lid or modified pens with a larger grip to customized wheelchair accessories to increase stabilization. Do not be afraid to use alternate items while practicing stabilization techniques and improving strength.
Another interesting facet of deficits following a cerebellar stroke is a disruption in vision. If you have had a stroke and note symptoms of vision changes, your vision as well as your visual perceptual skills should be evaluated by a neuro-ophthalmologist. You may require further referral by physical, occupational therapy, or a vision therapist with specialties in neuro-related vision deficits. Depending on the root of the problem, one or more of these specialties can provide special intervention and a home exercise program to improve fundamental visual skills to then attain greater functionality during movement and tasks of life.
Cerebellar strokes, although not as common as strokes of the middle cerebral arteries territories, treatment and recovery from the process provide their own challenges due to the nature of deficits that follow. Speak with your doctor or team member if concerns related to cerebellar function have not been addressed but are concerning and limiting function. Ask for referrals to therapy to address specific cerebellar deficits.
References:
Ng ZX, Yang WR, Seet E, Koh KM, Teo KJ, Low SW, Chou N, Yeo TT, Venketasubramanian N. Cerebellar strokes: a clinical outcome review of 79 cases. Singapore Med J. 2015 Mar;56(3):145-9. doi: 10.11622/smedj.2014195. PMID: 25820846; PMCID: PMC4371193.
Pendleton and Schulta-Krohn (2006) Pedretti’s Occupational Therapy Practice For Physical Dysfunction: 6th Edition. New York, Elisver.