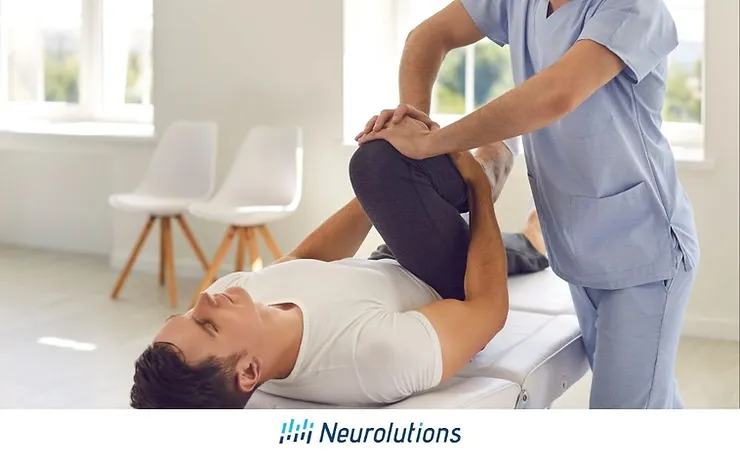
Recovering from a stroke usually involves participating in physical therapy (PT) and/or occupational therapy (OT), as well as follow-up medical care and social worker support. Physical and occupational therapy treatment plans for people who have recently experienced a stroke often include both passive and active exercises.
Even after a mild stroke, people can still experience weakness in an extremity, such as an arm or leg. Paralysis or weakness on one side of the body is among the most common of stroke impacts, interfering with normal daily activities.
In a research study led by Jayme S. Knutson, Ph.D, researchers found that 87% of stroke survivors experience some level of initial paralysis of the hand or upper limb (1). This not only limits independence for stroke survivors, but will affect family members, caregivers and personal health aids as well. However, the likelihood of a limb returning to pre-stroke functioning is increased if PT and/or OT is undertaken within the first three months following the stroke. This is attributed to the fact that the majority of progress in recovering motor skills (such as walking or self-feeding) occurs during that early post-stroke time period (2).
In comparison to PT, which is generally prescribed for treatment of the lower extremities, OT is generally prescribed for the upper extremities. Both physical and occupational therapists—whether in an outpatient office, rehab center, or patient’s home—use a variety of passive and active exercises to help the stroke survivor return to normal functioning. The following article describes the difference between passive and active exercises, as well as examples of these different categories of exercises and how they can be utilized in combination to foster better recovery outcomes.
What are Passive vs. Active Rehabilitation Exercises?
Passive Exercises:
Passive exercises performed within the context of PT and/or OT are those that are performed by the physical or occupational therapist on the body of the patient who has experienced a stroke or other type of brain injury. Depending on the severity of the stroke, the stroke victim generally experiences some paralysis or weakness typically on one side of the body. This is because a stroke in the left-side of the brain affects the right-side of the body, and a stroke on the right-side of the brain affects the left side of the body.
For stroke survivors who have experienced anything beyond a very mild stroke, both temporary or permanent paralysis of an upper or lower extremity is common. However, even a stroke that results in extreme weakness without actual paralysis can preclude self-performance of exercises that maintain the range of motion in the body’s joints.
The nerves in the brain frequently become damaged in a stroke, so the spinal cord nerves responsible for transmitting brain signals to muscle fibers to contract or relax become unable to send sufficient signals to the muscles. The consequence of the brain’s inability to transmit “instructions” to muscles via the spinal cord is usually paralysis or extreme weakness.
As nerve healing occurs in the brain, the paralysis or extreme weakness can begin to subside. However, muscles that are not used can lose their muscle tone, and the affected muscle fibers can lose their ability to contract and relax. This is why physical and occupational therapists perform passive exercises on the unused limbs that are unable to be moved by the stroke patient.
Due to the survivor’s inability to self-perform the necessary exercises, the physical or occupational therapist normally performs range-of-motion exercises and even electrical stimulation on the stroke survivor’s affected limb(s). This is initiated as part of the PT and/or OT treatment plan to preserve the capacity for the affected limb to potentially resume movement as the brain injury heals.
If range-of-motion exercises are not performed, muscles can tighten and become deformed into a set, or fixed, position. Also known as contractures, these can occur in the upper and lower extremities as well as the spine. In turn, this can destroy the capacity for future normal use and movement. When this happens in the hand, the person may never be able to pry open the paralyzed fingers due to the contracture- even if paralysis resolves.
For more information on management of hand and arm tightness following stroke, visit Flexor Synergy, Spasticity, and Stroke and How to Get your Hand Working after Stroke .
Active-Assisted Exercises:
Exercises that are actively performed by the stroke survivor and are partially supported by a helper, a device, or their own body are considered active assisted exercises.
For example, a stroke survivor may have some strength to raise their arm against gravity, yet they still need help to control the movement or to gain a greater range of motion. In this case, a therapist can support the elevation of the arm or the survivor can hold a cane in order to be guided by their stronger arm. They may use a mobile arm support device to unweight the arm to the desired preference to gain muscle strength.
Active Exercises:
Active exercises are PT and/or OT exercises that are typically performed by the stroke patient without assistance. These exercises can include range-of-motion exercises and strength-training. Range-of-motion exercises are aimed at maintaining or improving joint flexibility, while strength-training is often an aspect of the prescribed active exercises. Active exercises often incorporate movements that are used in performing the most common Activities of Daily Living (ADLs). This can include cycling on an exercise bike to boost knee flexibility and strength to prevent the likelihood of a stroke patient’s knees from “giving out”, or throwing rubber darts at a dart-board to exercise the finger joints.
How Can Exercises Help with Spasticity and Weakness in the Upper Extremities?
Following a stroke, new brain cells can develop to replace the damaged cells to aid the brain in healing. However, the biochemical “instructions” conveyed by the brain’s nerves to the spinal cord and muscles can still remain impaired even after the paralysis has ended. Therefore, the messages received by some of the muscles may still not be correct. The consequence of this impaired nerve signal transmission may be that the combined efforts of the various small muscles required for correct movement can be negatively impacted. This implies that muscles may move in a different or spastic way than desired. A pinky finger may wiggle when the thumb is moved, or bending the arm may cause the shoulder muscle to twitch. Weakness in the upper extremities can make bathing, self-feeding, dressing, or writing a letter very difficult.
Ultimately, the primary objectives of occupational therapy for stroke survivors who have overcome paralysis but are currently dealing with spasticity and weakness include: a) increase flexibility, b) increase strength, and c) enable performance as much as possible of that person’s normal activities.
What Are Passive Rehabilitation Exercises and How Do They Work?
Three examples of passive PT and/or OT exercises used in stroke rehabilitation are range-of-motion exercises, passive stretching, and electrical stimulation. In the upper extremities, the joints typically exercised to maintain range of motion are the shoulder, elbow, wrist, and finger joints.
For example, range-of-motion exercises for the wrist joint can be performed by flexing the wrist forward, backward, clockwise, and counter-clockwise as much as possible without injuring the joint. Neuromuscular Electrical Stimulation (NMES) can be used to assist with passive range of motion exercises during rehabilitation. NMES involves the use of electrical impulses to stimulate muscle contractions in individuals who may have difficulty maintaining joint flexibility. When used for passive range of motion, NMES helps move and stretch muscles and joints, preventing muscle atrophy and maintaining joint flexibility.
What Are Active Rehabilitation Exercises and How Do They Contribute to Recovery?
Enhance Mobility and Strength: Embrace Active Exercises
Active exercises typically include stretching, strengthening, and endurance exercises that the stroke patient performs entirely by themselves. The specific exercise is usually first modeled for the stroke patient by the physical or occupational therapist. This type of exercise promotes both flexibility and strength, as pressure is exerted on the elbow joint and the forearm muscles to stretch the exercise band into the therapist-requested position. A specified number of repetitions is then performed in accordance with the therapist’s instructions. In addition, the number of repetitions of the exercise tends to increase over the period of time in which the stroke patient is under the care of a physical and/or occupational therapist.
Boost Muscle Strength and Endurance in Stroke Rehabilitation
Muscle-strengthening exercises are often included in a stroke patient’s physical or occupational therapy regimen to improve muscle strength. In addition, exercise repetition to strengthen a muscle group and improve endurance is increased as the exercise becomes easier for the stroke survivor. Given that the motions integral to everyday ADLs typically take place numerous times, repetition holds great significance; an example of this can be seen in the act of raising a fork or spoon to the mouth while eating. Endurance in performing this activity needs to be fostered during PT/OT for a stroke survivor to successfully be able to perform ADLs, such as self-feeding.
Exercises categorized as active and active-assisted, which are aimed at promoting independence and performing ADLs, encompass a blend of exercise types such as range-of-motion exercises, muscle contracting/relaxing exercises, strength-building exercises, and endurance exercises.
Achieve Independence through Comprehensive Active-Assisted, Passive, Active, and Resistance Training
Stretching an arm above the head, throwing a ball, and lifting small weights are all exercises that an occupational therapist may include in an OT regimen to promote repetition and daily practice. Besides exercising during the PT and/or OT session, the stroke patient is typically provided with “homework” between sessions to perform daily range of motion and weight-bearing exercises. In addition to exercises targeted at muscle groups, occupational therapists can help stroke patients practice performing normal activities in order to support the patient’s capacity to return to pre-stroke functioning.
Should I Combine Passive and Active Exercises during Therapy Sessions?
Passive, active-assisted, and active exercises are all typically incorporated into a physical and occupational therapy treatment plan and are often utilized in combination with each other. By incorporating all of these exercise categories within a given treatment session, motor skill recovery in stroke and other brain injury patients may be expedited when compared to utilizing just one exercise category.
Enhancing Recovery Through Targeted Exercise Regimens
Passive, active-assisted, and active exercise can play a significant role in the recovery and independence of stroke survivors. Stroke often leads to physical and cognitive impairments, and regular exercise can help address many of these challenges.
Depending upon the motor skill impairment and cognitive impairments of the stroke survivor, the difficulty and complexity of the exercises and activities performed during PT and/or OT can be increased over time. The learning of new physical exercises can also boost cognitive skills.
By incorporating these skills and exercises, a stroke survivor can be well on their way to gaining independence, improving their mental well-being, and ultimately reclaiming their life post-stroke. As a reminder, the selection and implementation of all rehabilitation exercises should be approached with caution and under supervision to ensure safety and effectiveness.
References:
- Knutson JS, Harley MY, Hisel TZ, et al. (2007). Improving hand function in stroke survivors: A pilot study of contralaterally controlled functional electrical stimulation in chronic hemiplegia. Archives of Physical Medicine and Rehabilitation 88(4): 513-520. Webpage: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3961574/
- National Institutes of Health (NIH) [NIH Research Matters]. (September 28, 2021). Critical time window for rehabilitation after a stroke. Webpage: https://www.nih.gov/news-events/nih-research-matters/critical-time-window-rehabilitation-after-stroke
- De-Rosende-Celeiro I, Rey-Villamayor A, Francisco-de-Miguel I, et al. (2021). Independence in Daily Activities after Stroke among Occupational Therapy Patients and Its Relationship with Unilateral Neglect. International Journal of Environmental Research and Public Health 18(14): 7537. Webpage: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8306679/
- American Stroke Association (ASA). Depression and Stroke. Webpage: https://www.stroke.org/en/about-stroke/effects-of-stroke/emotional-effects-of-stroke/depression-and-stroke
- Thieme H, Morkisch N, Mehrholz J, et al. (2018). Mirror therapy for improving motor function after stroke. Cochrane Database of Systematic Reviews 7(7): CD008449. Webpage: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6513639/